Your neighbour was homebound six weeks ago. Couldn't get down the front steps without holding the railing. Now you watch them walk the beach every morning, barefoot, easy stride, no limp. You think: that can't be real. It looks too good to be true.
It is real. And it is, by almost every measure, one of the most successful surgical procedures in the history of modern medicine. Total hip replacement surgery — introduced to the world in 1962 by Sir John Charnley in Lancashire, England — has been quietly transforming lives for over sixty years. More than 55,000 Canadians have it done every year. The satisfaction rate sits at 94.4 percent. The implants last thirty years. The recovery, for most people, is faster and less painful than they imagined.
So why do so many people wait? Why do they manage the pain with anti-inflammatories and cortisone shots and a careful avoidance of stairs for years — sometimes a decade — before finally doing something about it? The answers are complicated: fear of surgery, fear of the recovery, a misplaced stoicism, and in Canada, a very real uncertainty about how long the wait will be.
This is the full teardown. What the surgery actually involves. What the wait looks like across the country. What it costs if you don't want to wait. What happens to your body if you keep delaying. And what life looks like on the other side — which, if the data is anything to go by, looks a great deal like your best days ever.
What They Actually Do
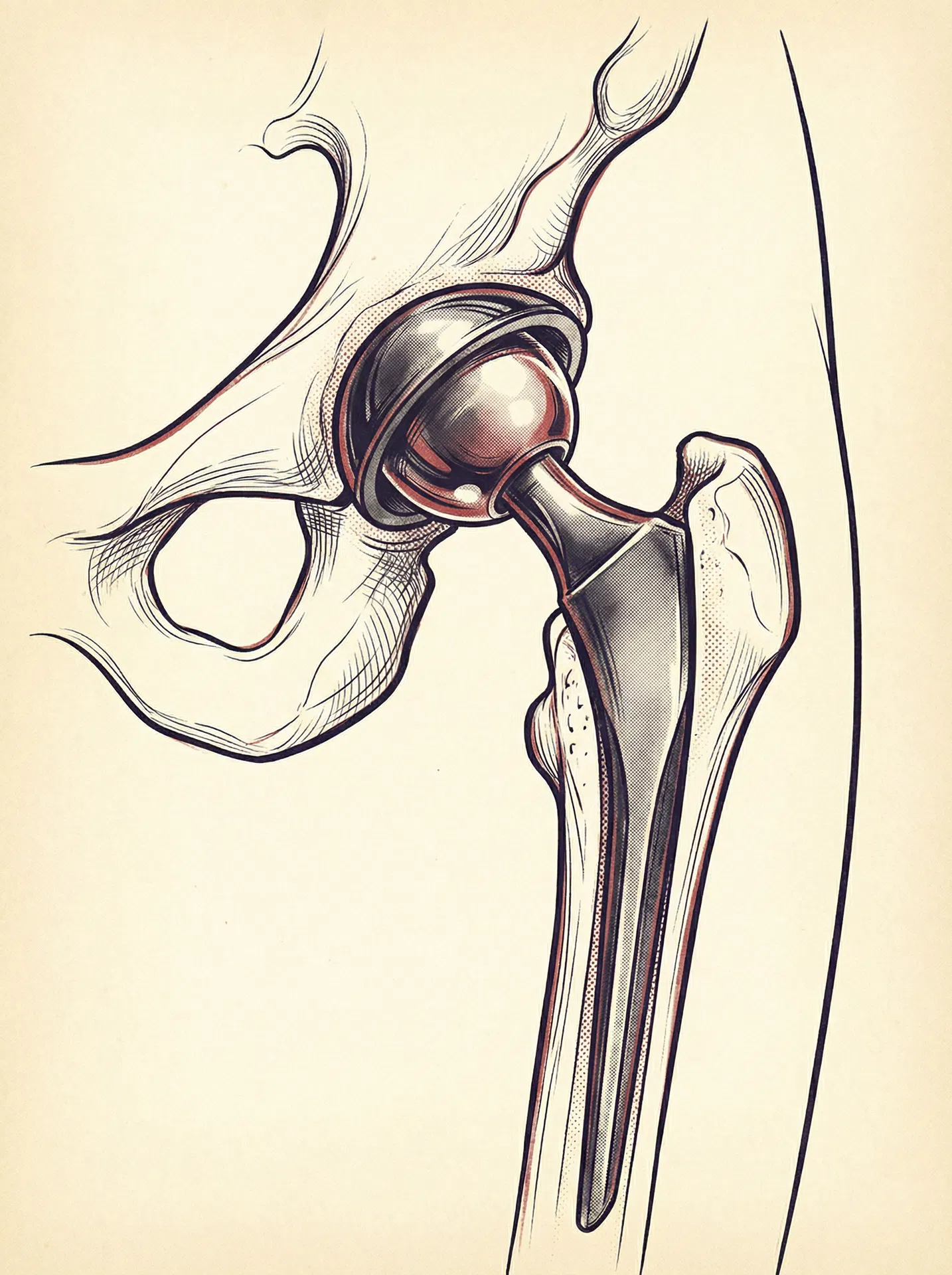
The hip is a ball-and-socket joint. The ball is the rounded top of your femur (thigh bone); the socket is a cup-shaped cavity in your pelvis called the acetabulum. In a healthy hip, both surfaces are covered in smooth cartilage that allows the joint to glide frictionlessly through its full range of motion. Osteoarthritis — the most common reason for hip replacement — gradually destroys that cartilage until you are, quite literally, bone on bone.
In a total hip replacement, the surgeon removes the damaged ball and socket and replaces them with a prosthetic implant. The femoral component — a metal stem — is inserted into the thigh bone with a polished ball on top. The acetabular component — a metal cup lined with ceramic or polyethylene — is fixed into the socket. The two components articulate together, recreating the smooth, pain-free movement your joint had before arthritis took hold.
The surgery takes one to two hours. You will be under general or spinal anaesthetic. Most patients spend just one or two nights in hospital. The physiotherapist will have you on your feet within four hours of the operation.
Front Door or Back Door?
There are two primary surgical approaches to hip replacement, and the debate between them is one of the livelier conversations in orthopaedic surgery. The posterior approach — incision at the back of the hip — has been the standard for decades. It offers excellent visibility for the surgeon and a strong track record. The anterior approach — incision at the front — is muscle-sparing, which means the surgeon works between muscle groups rather than cutting through them.
The anterior approach typically means faster early recovery, a reduced risk of dislocation, and fewer post-operative movement restrictions. A 2025 study in PMC found that both approaches yield equivalent functional results at three months and one year — so the long-term outcome is comparable. The difference is in the first few weeks: anterior patients tend to be more mobile, more quickly.
Ask your surgeon which approach they use and how many they perform per year. Volume matters. A surgeon who does 150 anterior hips a year will produce better outcomes than one who does 20. This is not a controversial statement — it is what the data shows.
Choosing Your Implant
The bearing surface — the materials that move against each other — determines how long your replacement lasts and how well it performs. This is a conversation worth having with your surgeon.
Most common; proven track record; plastic liner wears over time
Very low wear rate; excellent for those returning to sport
93% survival at 25 years; rare 'squeaking' risk; hardest wearing
Modern implants: 85–90% last 20+ years. Third-generation ceramic-on-ceramic implants show 93% survival at 25 years (Kaplan-Meier analysis, 2024). The hip replacements being implanted today could potentially last 30 years or more in moderately active individuals.
How Long Will You Wait?
Canada's national benchmark for hip replacement surgery is 182 days — 26 weeks. As of 2024, only 66% of patients receive their surgery within that window, down from 75% in 2019. The national median wait is approximately 131 days, which means half the country is waiting longer than four months. The numbers vary enormously by province.
What the table below does not capture is the experience of waiting — the cancelled plans, the worsening pain, the slow erosion of independence, the three-month window that becomes six months that becomes a year. The wait is not a neutral holding pattern. It is a period during which your joint continues to deteriorate and your muscles continue to atrophy.
| Province | Median Wait | Within Benchmark | Note |
|---|---|---|---|
| Ontario | 91 days~13 weeks | 79% | Best in Canada |
| British Columbia | 121 days~17 weeks | 70% | — |
| Alberta | 140 days~20 weeks | 65% | Rural areas: 42+ weeks |
| Manitoba | 154 days~22 weeks | 60% | — |
| Nova Scotia | 166 days~24 weeks | 55% | — |
| Quebec | 175 days~25 weeks | 55% | — |
| Newfoundland | 198 days~28 weeks | 50% | — |
| New Brunswick | 229 days~33 weeks | 45% | — |
| PEI | 231 days~33 weeks | 45% | — |
| Saskatchewan | 232 days~33 weeks | 40% | Longest in Canada |
Source: Canadian Institute for Health Information (CIHI), 2024 data. Benchmark = percentage of patients receiving surgery within the 182-day national standard.
The Cost of Not Waiting
Private hip replacement in Canada typically costs between $20,000 and $38,000 CAD — all-in, including surgeon's fee, facility, anaesthesia, standard implant, and post-operative follow-ups. It is not covered by provincial health plans. But it buys you a surgery date in weeks rather than months, a choice of surgeon, and a choice of implant. For many people, the calculation is straightforward. For others, the public system — despite its wait — delivers excellent outcomes at no direct cost.
| Option | Cost | Wait Time | Quality | Notes |
|---|---|---|---|---|
| Canadian Public System | $0 out of pocket | 13–33 weeks | Excellent | Covered by provincial health plan |
| Private Canada (major cities) | $20,000–$38,000 CAD | 2–6 weeks | Excellent | Not covered by provincial plans |
| Mexico (medical tourism) | $9,000–$29,000 USD | 1–4 weeks | Good–Excellent | Travel + accommodation extra |
| Thailand | $12,000–$14,000 USD | 1–3 weeks | Good–Excellent | JCI-accredited hospitals available |
| Hungary / Poland | $5,000–$12,000 USD | 1–4 weeks | Good | Lowest cost globally |
| United States | $40,000–$70,000 USD | 2–8 weeks | Excellent | Highest cost globally |
"A word on medical tourism: the headline numbers from Mexico, Thailand, and Hungary are real — but they rarely include flights, accommodation, the cost of a companion, or the very significant challenge of managing complications from 10,000 kilometres away."
Many Canadians who explore international options ultimately choose either the public system or a domestic private clinic for continuity of care and easier follow-up.
Recovery: Week by Week
A physiotherapist gets you upright and walking with a walker within hours of the operation. The arthritic pain that brought you here? Gone. There is surgical soreness — but that is a different thing entirely.
Most patients spend just 1–2 nights in hospital. You go home walking. Outpatient physio three times a week. Short walks, showers, basic independence restored.
By week two, most patients transition from walker to cane. By week four, many are walking unaided. Driving is typically cleared around the four-week mark.
Return to sedentary work. Begin swimming. Cook for yourself. The hip is doing what it was designed to do — and it is doing it without pain.
Pain is near zero. You can golf. You can hike. You can book the trip you have been putting off. This is the moment your neighbours were experiencing when you watched them walk the beach.
Return to your sport of choice — skiing, surfing, cycling, tennis. The hip is not a limitation. It is simply a joint that works.
Surgeons call it 'joint unawareness'. You will forget which hip was operated on. That is not marketing language. It is what 94% of patients actually report.

What Happens If You Don't
Osteoarthritis is a degenerative disease. It does not plateau. It does not stabilise. It worsens — at a rate that varies by individual, but worsens nonetheless. The cartilage continues to erode. The bone continues to grind. The inflammation continues to build. Every month you delay is a month the disease has to do more damage.
The physical consequences of delay are well-documented. Significant muscle atrophy begins months before surgery as pain forces you to reduce activity — and the weaker you are going into the operating room, the harder and longer the recovery. Your body compensates for the damaged hip by altering your gait, which transfers load to your back, your knees, and your opposite hip. Patients who delay surgery frequently arrive with secondary pain in three or four joints rather than one.
The fall risk is real and serious. A damaged hip reduces balance and coordination. Falls in adults over 65 are the leading cause of injury-related death in Canada. The opioid risk is also real: long-term management of hip pain with prescription opioids carries a well-documented risk of dependency, and patients who arrive at surgery having used opioids chronically have significantly worse outcomes and longer recoveries.
Then there is the life you are not living. The trips not taken. The grandchildren not chased. The morning walks not walked. The social withdrawal that comes with chronic pain — the dinners declined, the activities abandoned, the slow contraction of a life that was supposed to be expanding. A 2025 study of 149,774 patients found that 84.1% reported improved quality of life after surgery. Only 4.1% reported a worse outcome.
"The surgery is not the risk. The surgery is the solution. The risk is the years you spend managing pain while your joint, your muscles, and your life continue to deteriorate."
There is a timing consideration in the other direction too: surgeons generally recommend not having the operation too early, as artificial joints have a finite lifespan and a revision surgery is more complex than the original. The right time is when conservative treatments — physiotherapy, weight management, anti-inflammatories, cortisone injections — are no longer providing adequate relief and the pain is significantly limiting your daily life. That conversation belongs with your orthopaedic surgeon.
Too Good to Be True?
I watched my neighbour go from barely making it to the letterbox to walking the seawall every morning. Six weeks. I thought the same thing you probably thought: that can't be right. There must be a catch. There must be a harder story underneath the easy stride.
There isn't. The data is what it is. The satisfaction rate is 94.4 percent. The implants last thirty years. The recovery, for most people, is faster and less painful than they imagined. The catch — if you can call it that — is the wait. In Canada, that wait can be anywhere from three months to eight months depending on where you live. And during that wait, your joint is getting worse, not better.
The private option is expensive. Twenty to thirty-eight thousand dollars is not a small number. But it is also not an abstract number — it is the difference between waiting eight months in Saskatchewan and having a surgery date in three weeks. For some people, that calculation is easy. For others, the public system — despite its imperfections — delivers excellent outcomes at no direct cost, and the wait, while difficult, is manageable.
What I would say to anyone sitting on the fence: talk to your GP, get a referral to an orthopaedic surgeon, and have the conversation. The surgery is not the scary part. The scary part is the decade you might spend managing pain while your joint quietly gets worse and your best days quietly get fewer.
This article is for informational purposes only and does not constitute medical advice. Consult a qualified orthopaedic surgeon to discuss your individual circumstances.
Had Your Hip Done?
We want to hear from you. The good, the hard, the moment you realised it had worked. Your story could be the one that convinces someone else to stop waiting.
Share Your Story →
